Responding to the alarming rise in maternal mortality
This article appears in the 2019-2020 edition of CSG East’s Perspectives Magazine.

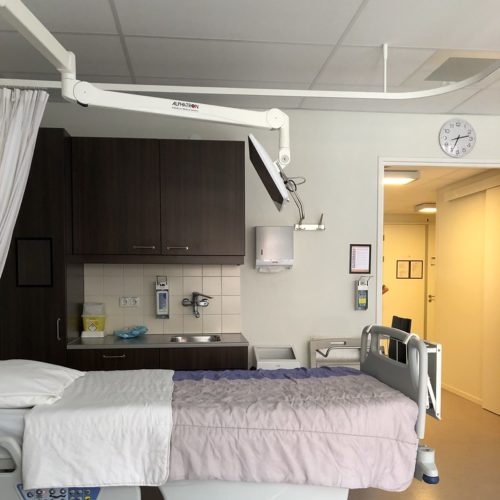
Health care panel participants during CSG/ERC’s 2019 Annual Meeting in Pittsburgh. From left: Lucy Hodder, J.D., Professor, University of New Hampshire School of Law; Tekisha Everette, Ph.D., Executive Director, Health Equity Solutions; Stacy Beck, M.D., Assistant Professor, University of Pittsburgh. Credit: Sebastian Marquez Velez
Last August, members of the CSG/ERC Health Committee gathered to discuss a startling fact about maternal health: More women die from pregnancy-related complications in the United States than in any other developed country, and the number of expectant mothers who die in childbirth is on the rise.
The group met with doctors, nurses, and state policymakers, who pointed to a range of factors contributing to the dangers for pregnant women, including lack of access to health care in rural communities as well as implicit bias and racism in the health care system.
“This work actually keeps me up at night, because I’m a mother myself,” said Lisa Asare, assistant commissioner for the New Jersey Division of Family Health, who participated in a panel discussion during CSG/ERC’s 2019 Annual Meeting in Pittsburgh.
As maternal mortality rates have increased in the United States, they have declined in other industrialized nations. According to a study in The Lancet, the maternal mortality rate in the United States in 2015 (26.4 deaths per 100,000 live births) was nearly three times higher than Britain’s and seven times higher than in Denmark or Finland. The Centers for Disease Control and Prevention (CDC) reported that about 700 women in the United States die from pregnancy-related complications each year, and alarmingly, 60 percent of these deaths could have been prevented. These statistics, along with recent, well-publicized experiences of several high-profile women who encountered life-threatening complications during childbirth — like Serena Williams — have forced policymakers to address this crisis, particularly among communities of color and rural communities.

Source: CDC, Morbidity and Mortality Weekly Report (MMWR), Racial/Ethnic Disparities in Pregnancy-Related Deaths — United States, 2007–2016.
Asare said that she works on multiple fronts to improve health outcomes in New Jersey, including empowering patients to seek medical help for conditions that could be life-threatening and improving the level of care that hospitals provide to pregnant women. For example, health care practitioners know that some of the leading causes of maternal mortality are hemorrhages and sepsis, but not every hospital has concrete protocols in place to deal with those conditions, said Asare.
Maternal Mortality Review Committees
One promising tool that has helped Asare and other health care professionals is state-based maternal mortality review committees (MMRCs). MMRCs are expert panels that investigate and review individual maternal deaths, then make recommendations and present actionable guidelines for community providers to prevent such tragedies. One of the most successful MMRCs is the California Maternal Quality Care Collaborative, an initiative begun in 2006 that helped California reduce its maternal mortality rates to a historic low today.
In 2018, Congress passed the Preventing Maternal Deaths Act, which created a grant program at the CDC to encourage states to adopt MMRCs or revitalize existing ones. In August 2019, the CDC awarded its first round of funding to support MMRCs in 25 states — including ERC member states Connecticut, Delaware, New Hampshire, New Jersey, New York, and Pennsylvania.
In Pennsylvania, simply accessing care during pregnancy has become a challenge in many communities, given a steady wave of closures among hospital obstetric units in recent years. From 2004 to 2014, nearly one-quarter of obstetric units across the state closed, according to figures from the state Department of Health, due to high maintenance costs and staffing shortages. It is not uncommon for women, particularly in rural areas, to have to drive up to four hours to receive maternal care, said Stacy Beck, an assistant professor in the Department of Obstetrics, Gynecology, and Reproductive Sciences at the University of Pittsburgh. Studies have shown a relationship between distance to obstetric care and poor medical outcomes. This problem is affecting rural communities across the country.
In fact, one of the biggest challenges for women everywhere is a persistent lack of access to even primary care. “In the United States, the majority of women only receive health care when they are pregnant, so a whole range of problems go unnoticed, like diabetes, and then we only have 10 months to try to fix those problems,” said Beck during the panel discussion in Pittsburgh. “As a physician, I often feel helpless.”
Breaking Down the Data
As chair of Pennsylvania’s recently formed MMRC, Beck is leading an effort to take a “systems-based approach” to determine which communities are most affected by poor care. Data is critical to understanding the “big picture” of maternal care — what is affecting women in every community of a state. But compiling data takes time. Beck’s team is reliant on doctors and coroners for medical records, which they can be reluctant to turn over. “For the first year of our maternal mortality committee, I felt like we were going around and begging people to release their data to us,” said Beck.
Once the data is collected, it is critical to break it down, to understand the subpopulations that fare the worst, said Tekisha Everette, executive director for Connecticut-based Health Equity Solutions, a nonprofit that promotes policies to advance health equity.
Connecticut is considered to be among the states with the best overall quality of health care, but it also has one of the highest levels of health disparities, said Everette during the panel discussion. Black women and Native American women in Connecticut are faring four to five times worse in maternal mortality outcomes than white and Latina women, she said.
Last year, Everette’s organization supported a Connecticut bill that would have given women in low-income communities better access to doulas, who assist women throughout their pregnancies and advocate for their health. Data shows that doula-assisted women are two times less likely to have a birth complication and four times less likely to have an underweight baby, said Everette. The bill, which failed to pass, would have created a state certification program for doulas and enabled them to get Medicaid reimbursements, as is done in Rhode Island and New Jersey. Minnesota, New York, and Oregon also provide Medicaid reimbursement for doulas.
Currently, a Connecticut state task force is exploring options for regulating and supporting doulas, with the aim of making recommendations to lawmakers for the upcoming legislative session. The hope is that providing women of color with greater access to doulas will help reduce the soaring rate of pregnancy-related deaths in their communities, said Everette.
In New Jersey, which has one of the oldest MMRCs in the country, Asare’s agency is exploring disparities in care among different communities and looking at issues around equity among providers. “We are really talking about implicit bias: how you look at other people and interact with them,” she said.
Other important factors that affect a woman’s level of care are the “social determinants of health” — which refer to the economic and social conditions in the places where people live and work that influence health risks and outcomes. “This is not just a health issue. It’s about so many other things: transportation, income, education — it’s about all of the things that feed into people’s day-to-day lives,” said Asare.
According to research by Review to Action, a partnership between the Association of Maternal and Child Health Programs and the CDC, only Maine, Vermont, and Rhode Island do not have a MMRC among ERC states.
CSG/ERC will continue to follow this important issue and provide updates on additional recommendations.
Insert:
According to a USA Today analysis of available maternal mortality data for 2016, Louisiana had the highest maternal mortality rate (58.1 per 100,000 births) and California had the lowest (4.0 per 100,000 births) in the United States. The following are the available results for ERC states.
| State | Ranking | Maternal deaths per 100,000 live births |
|---|---|---|
| Connecticut | 43 | 10.5 |
| Delaware | unavailable | unavailable |
| Maine | 28 | 18.9 |
| Maryland | 23 | 19.7 |
| Massachusetts | 45 | 8.4 |
| New Hampshire | unavailable | unavailable |
| New Jersey | 5 | 36.2 |
| New York | 25 | 19.2 |
| Pennsylvania | 31 | 18.6 |
| Rhode Island | 15 | 22.1 |
| Vermont | unvailable | unavailable |
*Source: USA Today